Summary
- Most hospice AI initiatives fail due to poor data readiness, not weak algorithms
- Fragmented EMR, referral, and payer data limits predictive accuracy
- AI readiness requires unified data, governance, and real-time integration
- High-impact use cases include referral automation, predictive care, and revenue integrity
- A data-first strategy is critical before investing in AI tools
Introduction
Walk into any hospice boardroom today and one topic dominates the agenda: AI.
From predictive analytics to workflow automation, hospice leaders are actively exploring how AI can solve staffing shortages, compliance pressure, and shrinking margins.
Financial pressure is becoming increasingly difficult for hospice providers to absorb. According to the latest reimbursement update from the Centers for Medicare & Medicaid Services, hospices received a 2.6% increase in Medicare base rate payments for 2026, slightly above the initially proposed 2.4% adjustment. While this translates to approximately $750 million in additional federal hospice spending, many providers continue to face rising labor, compliance, and operational costs that outpace reimbursement growth. The hospice aggregate payment cap also increased to $35,361.44 in 2026, reinforcing the need for organizations to improve efficiency, visibility, and financial control across care operations.
In this environment, hospice organizations are increasingly being asked to deliver better outcomes without proportional increases in reimbursement, making operational intelligence and data-driven efficiency critical priorities.
But there is a problem, most conversations overlook.
AI is only as effective as the data it runs on. And in hospice care, that data is often fragmented, inconsistent, and disconnected.
As leaders prepare for NPHI 2026 Summit, the real question is not which AI vendor to choose.
The real question is whether your organization is ready for AI at all.
Why Do Most Hospice AI Projects Fail?
Most AI failures in hospice do not happen after deployment. They happen before a model is even trained.
The root cause is data fragmentation.
Across many hospice organizations:
- Patient records exist across multiple EMRs and legacy systems
- Referral data remains locked in fax or unstructured formats
- Clinical documentation varies across caregivers
- Payer, operational, and care data do not connect
Individually, these issues seem manageable. Together, they create a system where AI models operate on incomplete and duplicated data.
This leads to a dangerous outcome.
AI does not simply produce wrong answers. It produces confident wrong answers.
In hospice care, that risk directly impacts patient outcomes, compliance, and revenue.

What Does AI-Ready Data Mean in Hospice Care?
AI readiness is not about buying technology. It is about building the right data foundation.
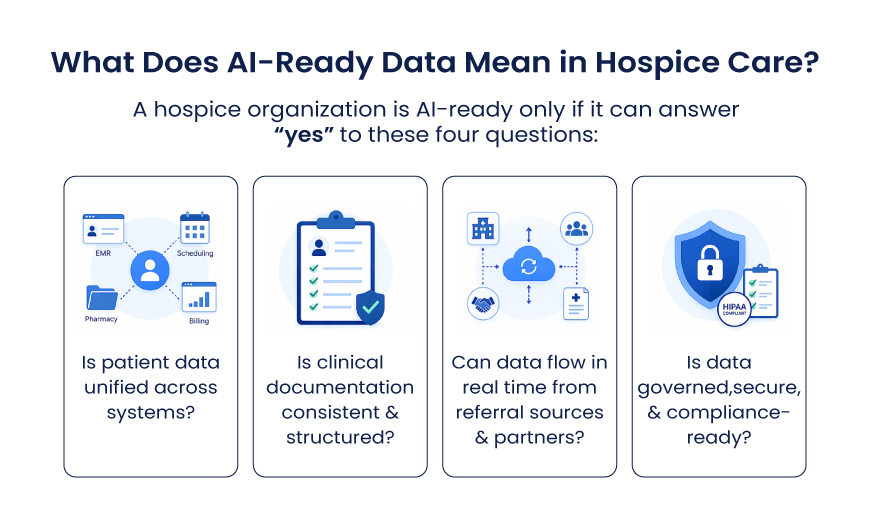
A hospice organization is AI-ready only if it can answer “yes” to these four questions:
- Is patient data unified across systems?
- Is clinical documentation consistent and structured?
- Can data flow in real time from referral sources and partners?
- Is data governed, secure, and compliance-ready?
This is where most organizations struggle. Not because they lack tools, but because they lack a connected data foundation.
In practice, leading organizations are moving toward a unified approach where clinical, operational, and financial data are brought together into a single layer before any AI is applied. Healthcare workflow automation platforms like Caregence are built around this principle, ensuring that AI operates on a consistent and reliable view of patients, workflows, and outcomes.
If any of these conditions are missing, AI investments will underperform regardless of the vendor or model quality.
What Data Challenges Prevent AI Adoption in Hospice?
Most hospice organizations do not lack data. They are lacking usable data.
Common challenges include:
- Duplicate patient records across systems
- Unstructured referral intake processes
- Siloed clinical, financial, and staffing data
- No real-time integration with hospital partners
- Manual compliance and audit workflows
These are operational bottlenecks that directly limit AI effectiveness.
Where AI Creates the Most Value in Hospice Operations
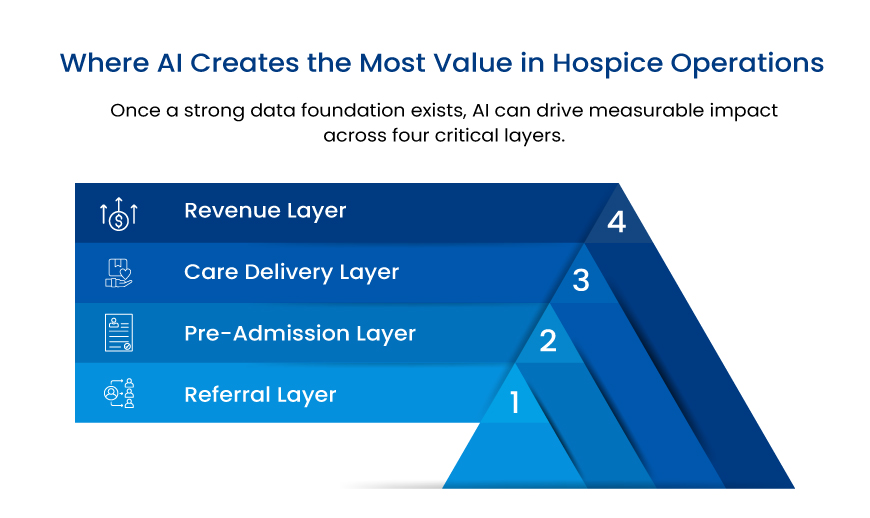
Once a strong data foundation exists, AI can drive measurable impact across four critical layers.
1. Referral Layer: Where Revenue Is Won or Lost
Hospitals are now a primary referral source. Speed is everything.
AI can:
- Convert referrals into structured data
- Score eligibility in real time
- Flag conversion risks early
Even small improvements here create significant impact at scale.
2. Pre-Admission Layer: Predict Before You Commit
AI enables better decision-making before admitting patients.
With clean data, models can predict:
- Length of stay
- Patient risk
- Cost alignment
This allows organizations to plan proactively instead of reacting later.
3. Care Delivery Layer: Proactive, Not Reactive Care
This is where AI begins to influence clinical outcomes.
Predictive models can:
- Detect deterioration signals
- Trigger timely interventions
- Support compliance with frameworks like HOPE
Care shifts from reactive to proactive.
4. Revenue Layer: Compliance and Financial Protection
Audit pressure is increasing across hospice organizations.
AI can:
- Align clinical and billing data
- Flag inconsistencies
- Generate audit-ready documentation
This reduces financial risk and strengthens compliance.
The Caregiver Equation: Why This Is Also a Workforce Problem
Most caregiver burnout is driven by friction, not compensation.
Scheduling inefficiencies, repetitive documentation, and disconnected tools reduce time spent on patient care.
A connected, data-driven environment can:
- Reduce administrative burden
- Improve onboarding
- Enable better caregiver-patient matching
Even a small improvement in retention creates significant financial and operational impact.
Case in point: Inferenz modernized a fragmented enterprise data ecosystem for a large healthcare organization, creating a unified digital front door that improved data accessibility, streamlined patient engagement workflows, and enabled faster, more coordinated care operations across systems through an enterprise data platform modernization initiative.
How Can Hospice Organizations Become AI-Ready?
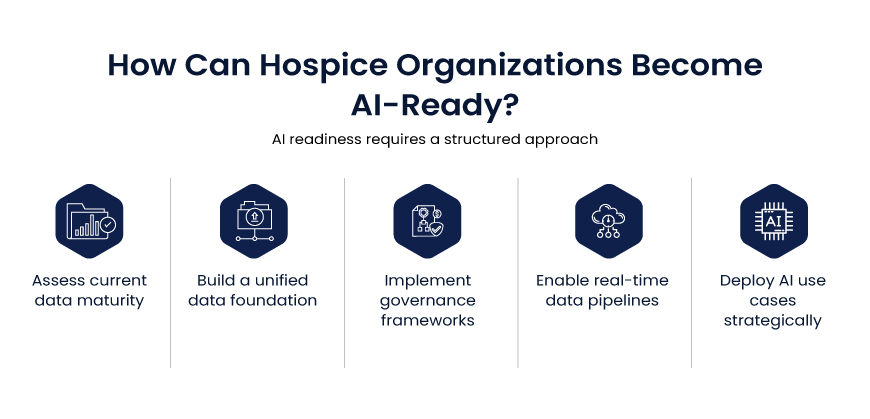
AI readiness requires a structured approach:
- Assess current data maturity
- Build a unified data foundation
- Implement governance frameworks
- Enable real-time data pipelines
- Deploy AI use cases strategically
This shift is already operationalized through healthcare-native platforms that unify data, workflows, and AI into a single ecosystem. AI-based workflow automation solutions like Caregence reflect this approach, helping organizations move from fragmented systems to connected, AI-ready operations.
Key Takeaways
- AI success depends on data quality, not algorithms
- Fragmented data is the biggest barrier to adoption
- Unified data enables predictive intelligence
- Compliance and governance are essential
- A data-first approach drives ROI
Conclusion: The Real Decision Hospice Leaders Must Make
Every AI investment will perform exactly as well as the data behind it.
Hospice leaders today face pressure across margins, compliance, workforce, and referrals. These are not separate challenges. They all stem from the same issue: fragmented data.
The decision is not which AI tool to implement.
The decision is whether to build the data foundation that makes agentic AI work.
Organizations that move toward a connected, data-first model will lead to the next phase of hospice transformation. Increasingly, this is being enabled through platforms that unify data, workflows, and intelligence into a single layer. Enterprise workflow automation solutions like Caregence represent what this future looks like in practice.

FAQs
What is AI readiness in hospice care?
AI readiness in hospice means your patient data is unified, deduplicated, and governed well enough for predictive models to trust it. That starts with resolving fragmented records across EMRs into a single patient view. Without it, any AI tool you deploy is making clinical and operational predictions on incomplete information.
Why does AI fail in hospice organizations?
Most hospice AI projects fail before a single prediction is made, not because of the algorithm, but because of the data underneath it.
Patient records spread across multiple EMRs, referral data trapped in fax format, and financial systems that never talk to clinical systems create a foundation that AI models cannot work from reliably. The result is confident predictions based on inaccurate inputs, which is worse than no prediction at all.
What are the top AI use cases in hospice?
The four highest-value areas are:
- Referral automation (converting fax-based intake into structured, scored records in real time)
- Predictive care planning (forecasting LOS, PPS progression, and deterioration risk before clinical decline)
- Staffing optimization (matching caregiver skills and geography to patient needs dynamically), and
- Revenue integrity (flagging GIP billing patterns that don’t align with clinical documentation before an audit does).
Each of these requires a clean, unified data layer to work accurately.
How can hospice leaders prepare for AI adoption?
Start with the data, not the model.
That means auditing your current EMR and RCM integrations for gaps, building real-time ingestion pipelines from referral partners and payers, implementing data quality and deduplication frameworks, and establishing governance controls that keep data HIPAA-aligned and CMS-compliant. Organizations that complete this foundation consistently get more from AI tools than those who deploy AI first and fix data problems later.
What role does compliance play in hospice AI?
Compliance is both a constraint and a driver.
CMS’s HOPE tool requires real-time, multi-visit clinical documentation with tight submission windows. Non-compliance risks a 4% Medicare payment reduction. An AI system built on governed, audit-ready data can automate HOPE scheduling, alert on missed Symptom Follow-Up Visits, and submit to iQIES within compliance windows.
In that context, compliance is one of the clearest ROI arguments for investing in it.


















